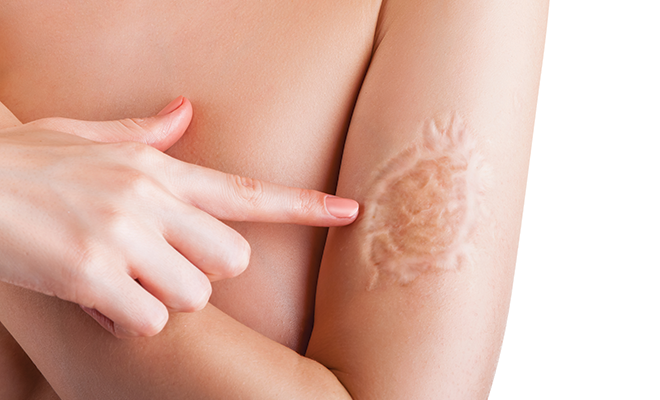
Don’t live with that scar
Remember when you were a little kid, and you fell and scraped your knee? Mom would kiss it and make it “all better.”
Although Mom’s gesture was comforting, the actual healing was part of our bodies’ near miraculous natural healing response, according to Jocelyn Ann Lieb, MD, FAAD, a board-certified dermatologist who practices at Advanced Dermatology P.C. and the Center for Laser and Cosmetic Surgery.
From that first bob-boo as a toddler to scars from a caesarean, accidents or other mishaps, probably no one goes through life without getting some kind of scar. Usually, this is no big deal, as many injuries heal without leaving much of a trace. But what about scars in visible places, such as on the face, or those that don’t eventually fade away?
A scar forms when there has been damage to the deep, thick layer of skin called the dermis, Dr. Lieb explains. As the skin heals, the new collagen fibers that replace the damaged tissue have a different protein composition than the original tissue, which causes the new skin to have a different texture and appearance than surrounding skin.
Most scars are flat and pale. When too much collagen is produced, the scar may be red and raised (hypertrophic) and if the raised scar extends beyond the boundaries of the original wound, it is known as a keloid scar. Contracture scars result from burns; as they tighten, they can restrict movement and may affect underlying muscles and nerves. Cystic acne and chickenpox scars are often pitted or indented (atrophic).
Dr. Lieb said the appearance of a scar depends on the size and depth of the wound, as well as the person’s age, genes and skin pigmentation. “But some disfiguring scars do not fade and cause emotional and physical discomfort long after the initial wound has healed. Fortunately, we can take steps to reduce the severity of a scar, and, although we can’t always remove it entirely, we have a range of treatments that can minimize the scar and make it more consistent with surrounding skin.”
For mild and shallow scarring, such as acne, cover-ups may do the trick as our skin heals. There are many brands of makeup for this purpose, including Dermablend®, which is a thick cream foundation and setting powder.
“If, despite your best efforts and the passage of time, you are still bothered by the appearance of a scar, your dermatologist can suggest a course of treatment appropriate for the severity and characteristics of the scar,” says Dr. Lieb. “Options range from topical applications to surgery.”
A silicon-based gel or a silicon gel sheet that is pressed on the skin can help flatten a swollen, raised scar. Silicon gel sheeting can also be helpful as the wound is healing, leading to a thinner, softer, less red and less painful scar.
Injections of corticosteroids are used to soften and flatten keloid and hypertrophic scars. Filler injections can raise sunken scars to the level of surrounding skin. To improve the appearance of a raised scar, dermabrasion and laser therapy are different methods that achieve similar results, removing the surface layers of the skin.
Surgery can alter a scar’s shape or make it less visible. The scar may be removed completely and the new wound closed carefully (excision) or a series of small incisions can re-orient the scar so it better follows the natural folds of the skin and is less noticeable (Z-plasty). A skin graft may be used when a large area of skin has been lost.
For keloid or any scars that are resistant to corticosteroid injections, there is a new procedure, Cryoshape, which freezes the keloid from the center and causes all or most of it to fall off. It is not yet covered by insurance.
“Any injury or trauma to the skin can cause a scar,” Dr. Lieb concludes. “If it is small or can be easily concealed, a scar may not be troubling. But for those that make people self-conscious and cause emotional distress, we can take steps to minimize the effects.” HLM
Source: advanceddermatologypc.com.